Retinoscopy Guide: Techniques & Applications for Optometrists
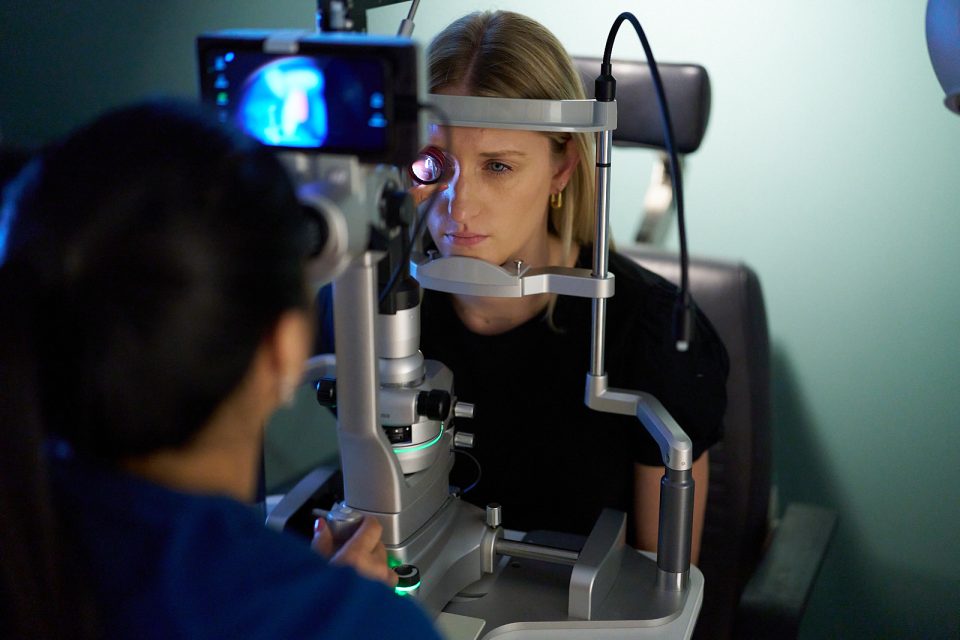
Retinoscopy is an eye test in which optometrists find and measure refractive errors using special tools to see how light travels through the corneas and lenses of your eyes and reflects off your retinas. When the light is bright and direct enough, the reflection causes a glow in your pupils that experts call the “fundus reflex” or “red reflex.”
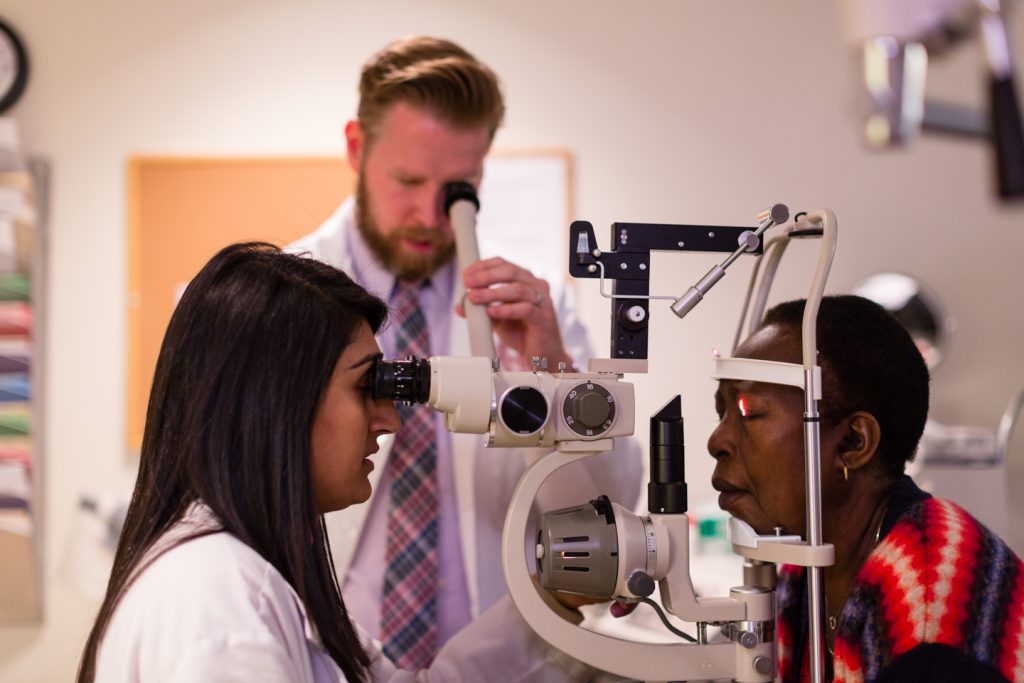
Through this light reflecting in the pupil, providers can diagnose diseases like myopia, hyperopia, or astigmatisms. At New England College of Optometry (NECO), students develop proficiency in this foundational technique before entering a clinical setting. Whether working with pediatric patients, individuals with communication barriers, or those who cannot provide subjective responses, retinoscopy remains a vital tool for optometrists in various clinical settings.
Let’s get Technical
When you have 20/20 vision, light rays bouncing off your retinas–also known as light reflex–should line up so they’re parallel when they leave your eyes. But if you have a refractive error, the error bends those rays differently, causing some of them to misalign. An optometrist may use the process of neutralization to find which vision corrections make the light rays align correctly. Those corrections become your prescription glasses.

Retinoscopy techniques include two ways to capture information: static and dynamic. Static retinoscopy is performed when the patient is fixating on a distant target, providing an objective measure of their refractive state at rest. Dynamic retinoscopy is when the patient focuses on a near target, often used to assess accommodative function and binocular vision.
Applications of Retinoscopy
Retinoscopy applications are important across all areas of optometric specialties. The test is particularly useful in pediatric optometry–where patients may not be able to provide reliable responses to refraction testing–and treating non-verbal or special needs patients who require more objective testing in order to provide clear responses.

Further, retinoscopy can provide additional insight into irregular astigmatism, often encountered in keratoconus or post-surgical corneas, and for early detection of amblyogenic risk factors such as high hyperopia, myopia, and astigmatism. By integrating retinoscopy into daily clinical practice, NECO ensures that graduates are well-equipped to provide comprehensive and accurate refractive care, even in challenging cases.
Despite advancements in the optometric field, retinoscopy remains an invaluable skill for optometrists. Its ability to provide real-time, objective refractive assessments makes it a crucial tool in a wide range of clinical scenarios. Through rigorous training and hands-on experience, NECO continues to prepare future optometrists to master retinoscopy and deliver high-quality eye care to diverse patient populations.